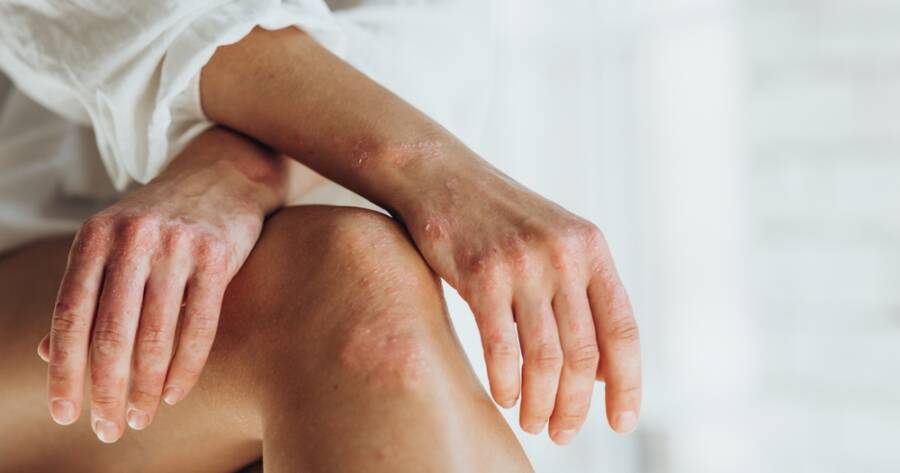
Psoriatic arthritis (PsA) is a chronic autoimmune condition that affects both the skin and joints. PsA typically affects people who have psoriasis, a skin condition that causes red, scaly patches on the skin. However, it can also occur in individuals who don’t have visible skin symptoms of psoriasis, making it challenging to diagnose and manage. Understand the complexities of psoriatic arthritis, its symptoms, causes, risk factors, and available treatment options.
What Is Psoriatic Arthritis?
Psoriatic arthritis is a form of inflammatory arthritis that occurs in some people who have psoriasis, though not everyone with psoriasis will develop PsA. The condition involves the immune system attacking the body’s tissues, causing inflammation and damage to both the joints and the skin. The joints, particularly in the hands, feet, knees, and spine, become inflamed and painful. PsA can lead to joint damage and deformities if not properly managed, and in some cases, it may result in reduced mobility.
Symptoms of Psoriatic Arthritis
The symptoms of psoriatic arthritis can vary widely from person to person, but they generally include both joint and skin manifestations. Some of the most common symptoms of PsA are:
- Joint pain and stiffness: This is the hallmark symptom of PsA. It typically affects the smaller joints in the hands and feet but can also impact larger joints like the knees and hips. The pain may be constant or come and go, and it can be aggravated by movement or inactivity.
- Swollen joints: Swelling around the affected joints is common in PsA. The swelling may be warm to the touch, and it can be accompanied by redness and tenderness.
- Skin changes: People with PsA often have psoriasis, which manifests as red, scaly patches of skin. These patches can appear anywhere on the body, but they are commonly found on the scalp, elbows, and knees. The skin lesions may worsen during periods of active arthritis.
- Fatigue: Many people with PsA report feeling unusually tired or fatigued, even if they haven’t been physically active. This can be due to inflammation and the body’s immune response.
- Nail changes: Psoriasis can affect the nails, causing pitting (small depressions), thickening, or discoloration. Nail involvement is common in PsA and may be an early sign of the disease.
Causes and Risk Factors
The exact cause of psoriatic arthritis is unknown, but it is believed to be the result of a combination of genetic, immune, and environmental factors. A malfunction in the immune system leads to inflammation in the joints and skin.
- Genetics: A family history of psoriasis or psoriatic arthritis increases the likelihood of developing the condition. Specific genes, such as the HLA-B27 gene, have been linked to an increased risk of PsA.
- Immune system dysfunction: PsA is an autoimmune disease, meaning the immune system mistakenly attacks the body’s tissues. In the case of PsA, the immune system targets healthy joint tissues and the skin, leading to inflammation and damage.
- Infection or injury: In some cases, infections or injuries may trigger the onset of PsA in individuals who are genetically predisposed to the condition.
- Environmental factors: Certain factors, such as stress, smoking, and obesity, may trigger or worsen PsA flare-ups.
Treatment Options for Psoriatic Arthritis
While there is no cure for psoriatic arthritis, there are effective treatments that can help manage symptoms, control inflammation, and slow the progression of the disease. Treatment for PsA typically involves a combination of medications, lifestyle changes, and sometimes physical therapy.
- Nonsteroidal anti-inflammatory drugs (NSAIDs): These medications, such as ibuprofen or naproxen, can help reduce pain and inflammation.
- Disease-modifying antirheumatic drugs (DMARDs): DMARDs, such as methotrexate and sulfasalazine, are used to slow the progression of PsA and prevent joint damage.
- Biologics: Biologic drugs, such as TNF inhibitors (e.g., adalimumab, etanercept) and IL-17 inhibitors (e.g., secukinumab), are used in cases where PsA is moderate to severe. These medications target specific components of the immune system involved in inflammation.
- Corticosteroids: In some cases, oral or injectable corticosteroids may be used to control inflammation during flare-ups.
- Topical treatments for skin symptoms: For psoriasis, topical treatments such as corticosteroids, vitamin D analogs, and moisturizers can help manage skin lesions.
- Physical therapy and exercise: Regular exercise and physical therapy can help maintain joint flexibility, reduce pain, and improve overall quality of life.
Living with Psoriatic Arthritis
Living with psoriatic arthritis can be challenging, but with the right treatment plan, individuals can manage the symptoms and lead an active, fulfilling life. It’s essential to work closely with a healthcare provider to monitor the condition, adjust treatment as needed, and manage flare-ups.
Making lifestyle changes such as maintaining a healthy weight, quitting smoking, and managing stress can also help improve outcomes. Regular check-ups with a rheumatologist or dermatologist are important for ongoing monitoring and care.
Managing Psoriatic Arthritis for a Better Quality of Life
Psoriatic arthritis is a complex and chronic condition that affects both the joints and the skin, leading to pain, inflammation, and reduced quality of life. While there is no cure, advancements in treatments such as biologics and DMARDs have significantly improved the management of the disease.
Early diagnosis and personalized treatment are crucial in managing PsA and preventing long-term joint damage. With the right care, individuals with psoriatic arthritis can lead fulfilling lives and manage the challenges of this condition effectively.